Birth control is something that can have a huge influence on your life. Now, I’m not here to tell you to be or not to be on any sort of birth control – that is completely up to you. I am here to at least give you the options and information that are available. I also strongly recommend speaking to the women who are close to you; you can get their experiences with certain contraception methods, but keep in mind, contraception affects us all differently.
This map shows all sexual health clinics, so you can find the closest place for help: Sexual Health Clinics.
You can also find help on the NHS website: Find a sexual health clinic – NHS
Contraception is free and confidential, including for young people under the age of 16 – the doctor, nurse or pharmacist won’t tell anyone, including your parents or carer, unless they think you or someone else is at risk.

Condoms are typically 82% effective at preventing pregnancy; if used perfectly, they’re 98%. They have no effect on your period as they’re only used during sex. They do have the added bonus of preventing STDs and STIs. I would personally advise using condoms in all sexual encounters, whether you use any other form of contraception or not, just to stay safe against STIs. There are instructions on the packet to put a condom on correctly, also make sure your condom isn’t expired, as it may not be as effective. You can get free condoms at any sexual health clinic and some GP surgeries. You can also buy them at most supermarkets.
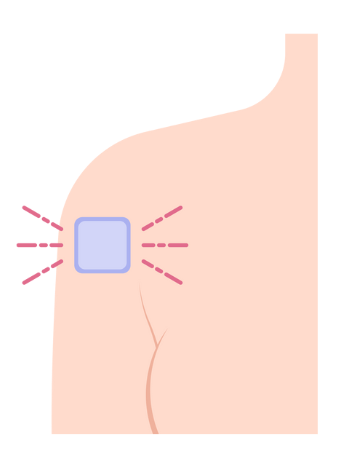
The patch is a small square that you wear on your skin. If worn correctly 100% of the time, it is 98% effective at preventing pregnancy. It releases the hormones oestrogen and progesterone into the blood, which stops your ovaries from releasing an egg each month. You wear it for 7 days and then replace it with a new one. You may experience some side effects: bleeding between periods or changes to your periods, headaches, feeling sick or dizzy, or sore breasts. It can also cause high blood pressure in a small number of people. You can get the patch at any sexual health clinic and some GP surgeries.

The pill is a type of hormonal contraception containing oestrogen and progestogen that prevents an egg from being released from the ovaries each month. It’s over 99% effective if used correctly; however, if you miss a pill, for example, it’s less effective. You have to take the pill once a day, at roughly the same time every day. The pill can help with acne, heavy or painful periods, and endometriosis. You may experience some side effects: bleeding between periods or changes to your periods, headaches, feeling sick or dizzy, or sore breasts. It can also cause high blood pressure in a small number of people. Taking the pill can also slightly increase your risk of getting breast cancer or cervical cancer. You can get the pill from sexual health clinics, GP surgeries and some pharmacies.
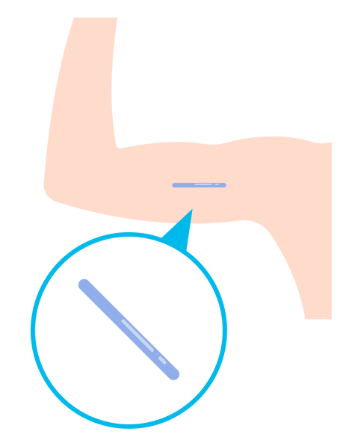
The implant is a small plastic rod that a doctor or nurse puts under the skin of your arm. It’s over 99% effective. It prevents pregnancy by releasing the hormone progestogen, which stops the ovaries from releasing an egg each month. The implant needs to be replaced every 3 years by a doctor or nurse. The most common side effect of the implant is a change to your periods. They may be more irregular or unpredictable, heavier or more painful, last longer, or stop completely. Other side effects can include headache, sore breasts, weight gain, acne and thrush. You can get the implant from sexual health clinics and some GP clinics. I personally have been on the implant since I was 15, and I’ve never had any problems with it; my most common side effect is unpredictable periods.
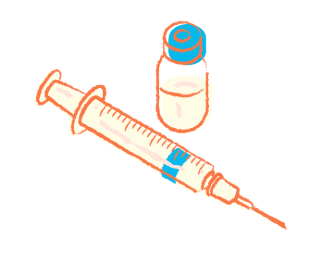
The injection contains the hormone progestogen, which prevents the ovaries from releasing an egg. It is over 99% effective; if you get your injection late, it’s less effective. The injection is given by a doctor every 8 to 13 weeks, depending on the type. Side effects include: changes to your periods, like them stopping, being irregular or lasting longer; putting on weight; and pain, a small lump or scar where the injection is done. Some people also report acne, lower sex drive, mood changes, hot flushes and headaches. You can get the injection at any sexual health clinic and some GP surgeries.
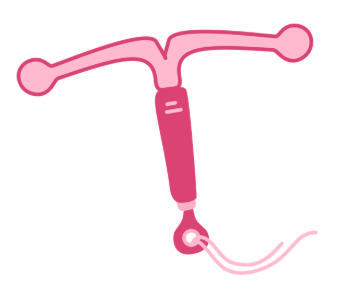
The IUD (intrauterine device) or copper coil is a small, plastic T-shape that a doctor or nurse puts into your womb. It doesn’t use hormones; it stops pregnancy by releasing copper into the womb. It’s over 99% effective and can last for 5 or 10 years, depending on the type. The IUD can also be used as an emergency contraception, as long as it’s inserted within 5 days after sex. It can be fitted by a trained doctor or nurse at a GP surgery or sexual health clinic. This is a lot more invasive procedure in comparison to the other forms of contraception. After you get an IUD fitted, you might have some period-like pain for a few days, some bleeding between periods, or your period might become heavier, longer, or more painful. You have a small chance of getting recurring thrush – talk to your GP if this happens. You can get the IUD fitted at any sexual health clinic and some GP surgeries.
The emergency contraceptive pill (morning-after pill) is an emergency contraception, not something you should take regularly as birth control. It can stop a pregnancy after sex without contraception, or if contraception fails. It needs to be taken within 72 hours after sex; the sooner you take the pill, the sooner it will work. You can get the pill from most sexual health clinics, GP surgeries and pharmacies. Common side effects include: headache, feeling sick and period-like pain or cramping. If you vomit within 2 hours of taking the pill, you may need to take another dose. You can speak to a pharmacist if you need help.
Leave a comment